
Why the DSM May Never Be Enough
Mental health diagnosis has long relied on structured systems like the DSM (Diagnostic and Statistical Manual of Mental Disorders). But what if the problem isn’t that the DSM needs improvement—but that the entire idea of rigid diagnostic categories is flawed?
A new line of thinking in mental health science suggests exactly that. Instead of treating disorders as fixed categories, researchers are proposing a more flexible, data-driven approach based on something called homeostatic property clusters (HPCs).
Let’s break down what this means—and why it could reshape public health, clinical care, and mental health policy.
The Problem With Current Mental Health Diagnoses
For decades, psychiatry has struggled with a core issue: mental disorders don’t fit neatly into boxes. Here are some of the biggest challenges:
- High comorbidity: People often meet criteria for multiple disorders at once
- Heterogeneous symptoms: Two people with the same diagnosis can look completely different
- Low reliability: Clinicians don’t always agree on diagnoses
- Limited clinical utility: Diagnoses don’t always guide treatment effectively
Despite multiple updates since 1980, these problems persist. The DSM, while useful, has been compared to a “paper plane held together with tape”—functional, but fundamentally fragile.
What Biology Can Teach Us About Mental Health
To understand the future of psychiatric classification, researchers are looking to an unexpected place: biology.
For centuries, biologists have also struggled to classify living things. Early approaches assumed species were fixed “natural kinds” (like elements in chemistry). But this turned out to be wrong. Instead, modern biology sees species as messy, evolving groupings with:
- No single defining feature
- Overlapping traits
- Blurry boundaries
For example, some animals we call “fish” are actually more closely related to mammals than to other fish.
Sound familiar?
The Big Idea: Mental Disorders as “Property Clusters”
The Homeostatic Property Cluster (HPC) model applies this biological insight to mental health. Instead of viewing disorders as fixed categories, the HPC approach sees them as:
Clusters of related properties that tend to occur together—but not always.
These properties include:
- Symptoms (e.g., sadness, anxiety)
- Biology (e.g., brain function, hormones)
- Behavior (e.g., sleep, substance use)
- Social factors (e.g., income, trauma, relationships)
- Psychological traits (e.g., personality, coping style)
Key Insight:
These features are probabilistically related, not deterministic.
- Poor sleep → often leads to low concentration (but not always)
- Trauma → increases risk for depression (but not always)
This creates fuzzy clusters, not clean categories.
Why Mental Health Is Inherently “Messy”
Under the HPC framework, the problems with diagnosis aren’t failures—they’re expected. Mental health exists in a complex, multidimensional space where:
- People cluster into overlapping groups
- Boundaries between disorders are unclear
- Many different pathways lead to similar outcomes
This explains why:
- Depression and anxiety often co-occur
- Treatments work across multiple diagnoses
- No single cause explains most disorders
In short: mental health doesn’t organize itself into tidy boxes—so our systems shouldn’t expect it to.
A New Vision: The “Mental Health Atlas”
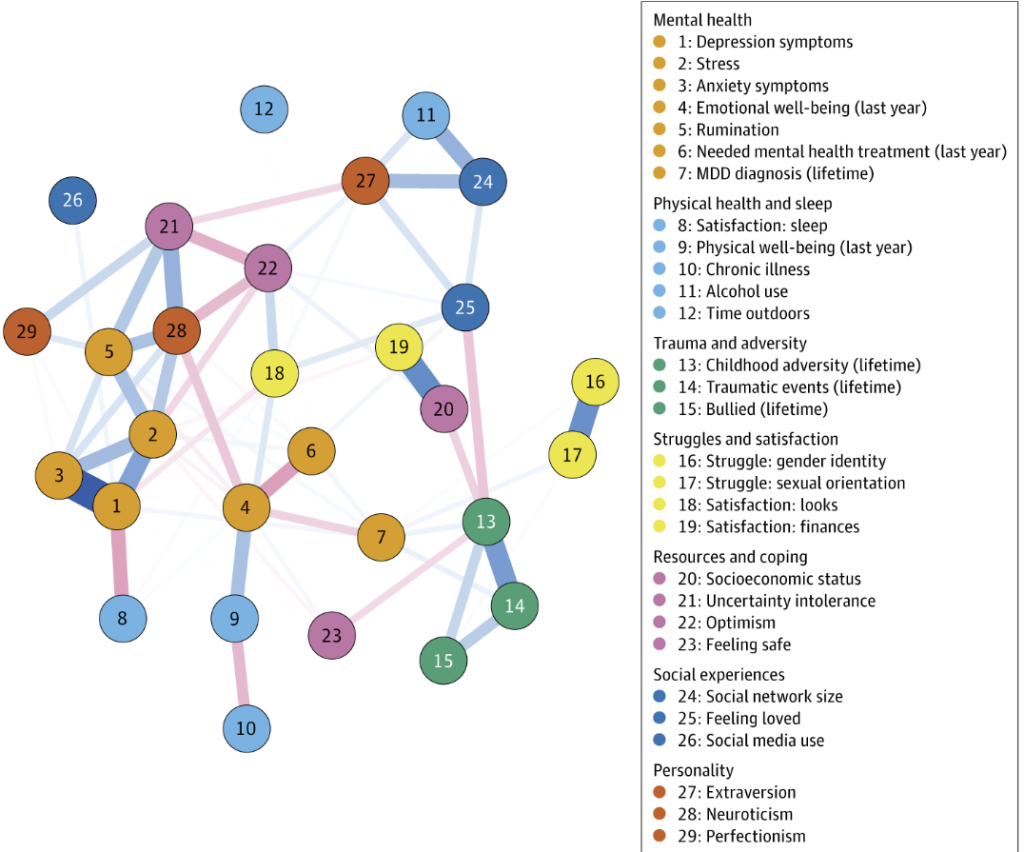
Instead of forcing people into categories, researchers propose building a “mental health atlas.” Think of it like a dynamic map that:
- Tracks thousands of mental health-related variables
- Shows how they cluster and interact
- Follows how individuals move through this space over time
What This Enables:
- Personalized care based on individual profiles
- Identification of shared mechanisms across disorders
- Better understanding of risk and resilience pathways
- Real-time monitoring using smartphones and wearables
This approach aligns with major public health frameworks, including:
- The biopsychosocial model
- Systems and network approaches
- Transdiagnostic treatments
Why This Matters for Public Health
This shift isn’t just academic—it has real implications.
1. Better Targeting of Interventions
Instead of treating diagnoses, we can target specific processes (like sleep, stress, or social isolation).
2. More Equitable Mental Health Systems
By including social and environmental factors, this model better captures structural determinants of health.
3. Improved Policy Design
Different stakeholders—clinicians, insurers, researchers—can use different classification systems tailored to their needs.
4. Moving Beyond “One-Size-Fits-All”
No single system will work for everyone—and that’s okay.
The Bottom Line
The HPC model challenges a core assumption in mental health: Diagnoses are not discoveries—they are decisions.
They are tools we impose on a complex reality, not truths waiting to be found. And that realization may be the key to finally moving forward.



